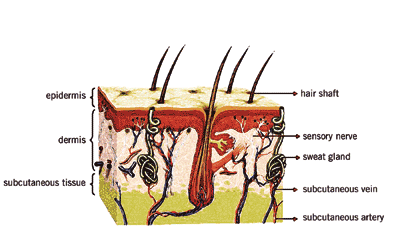
Jagdish Singh devotes many of his waking hours to searching for clever ways to penetrate a formidable barrier: the layer of dead skin cells covering the human body. The outer shell of densely packed cells, which under a microscope resembles a hound's-tooth coat of interlocking shingles, forms a natural suit of armor against invaders. That protective mechanism, which evolved over millennia, is good if the attackers are harmful bacteria or toxins in the environment. But it's an obstacle if the intruder is a dose of medicine. Medical science has long had an answer, of course, for piercing the body's outer wall: the needle. The hypodermic syringe is more than a prickly nuisance, however, for patients who must cope with diabetes. Diabetics must carefully monitor their blood-sugar levels and take insulin shots - sometimes multiple shots - daily. Failure to take their shots when needed can cause serious illness. Or even death.
Singh, a professor of pharmaceutical sciences at North Dakota State University, is working with colleagues to develop a better way for diabetics to receive insulin: by absorption, instead of injection. True, it's now commonplace for smokers trying to kick the tobacco habit to wear a nicotine "patch," and some birth-control therapies can be delivered in the same painless manner. But there's a problem. The handful of drugs that so far can be administered via the skin patch involve medicines comprised of small molecules. Insulin, on the other hand, is a polypeptide hormone, an elephantine molecule of amino acids that can't pass through the skin's small doorways without lots of sophisticated manipulation. Or, as Singh says, with a scientist's penchant for dry understatement, "The delivery of the big molecules is a problem."
To enable those ungainly insulin molecules to sneak past security, Singh is working to perfect a technique, called iontophoresis, which combines two steps. First, it uses what are called chemical enhancers to enlarge the openings in the skin by extracting fats and proteins that are part of the protective top layer of skin cells. Then, with the door chemically opened, a very mild electrical current is employed to push the insulin through the doorway. The nudge comes from repulsion created by two identically charged electrical electrodes in a device that looks much like a wristwatch. (Singh's work involves the chemical and biological processes of drug delivery; others are developing the device.) So far, Singh's research has produced promising early results in tests involving rabbits and pigs that have been induced to develop diabetes. Animal subjects have received adequate doses of insulin without showing adverse side effects. "We find very encouraging results," Singh says. Someday, he adds, "We have to see whether it will cause skin irritation in humans. In animals it has not."

More animal tests are needed, however, before clinical trials involving human patients can begin. His research to date has been funded by the prestigious National Institute of Child and Human Development. Singh has applied for additional funding from the National Institutes of Health to continue testing. He hopes clinical trials can begin in two or three years. Singh brims with optimism based on the results so far, and the technique's demonstrated success. "I don't see any reason why it shouldn't work," he says. He has published results of his foundational research - Singh has published more than 100 peer-reviewed research papers, reviews and book chapters in his career - and the pharmaceutical industry is eagerly watching to see what develops. "I think money is going to start flowing in this direction."
Dr. Juan Munoz, an endocrinologist at MeritCare Clinic in Fargo, has been following Singh's work, and has agreed to participate in the clinical trials. He's impressed with the early results and, like Singh, convinced that the technique is sound. If successful, delivering insulin by means of an "insulin watch" would be a great improvement over the pincushion therapy of daily injections - especially among patients who hate shots, or those who forget to take shots on schedule. Munoz says he's encouraged by the early animal tests; both rabbits and pigs have thicker, tougher skin than people do, he notes. "If it works for rabbits and pigs, it should work for people," Munoz says. Other new means of delivering insulin - including a nasal spray - are flawed because it is difficult to reliably administer an adequate dose, Singh says. And an "insulin watch" could deliver a dose over a longer period of time for patients with acute diabetes.
Meanwhile, on another research track, Singh is working toward developing gene therapies that he hopes someday will prevent diabetes in people who are genetically susceptible, such as American Indians, who have much higher rates of diabetes than the general population. He is working with two doctoral students on a therapy that would use plasmid-DNA supplied by Aldevron - a Fargo biotechnology firm founded and heavily staffed by NDSU graduates - and Interleukin-10, a protein made in the body that stimulates the immune system. The idea would be to prevent damage to the pancreas, the gland that produces insulin, a vital hormone that enables the body to regulate sugar and other carbohydrates.
Singh's initiatives to treat and perhaps even prevent diabetes are part of a broader body of research aimed at developing novel techniques for delivering drugs - a quest that began almost by accident. Originally, when growing up in Varanasi, a large city in northern India near the Ganges River, he wanted to be an engineer. Then, during his undergraduate studies, he developed an interest in biology, and considered medicine. Ultimately he decided he would be a research scientist who would develop new medicines instead of practicing medicine. His earliest work involving skin absorption therapies began at the University of Otago in New Zealand, studying under Michael S. Roberts, an acknowledged leader in the field. He continued his studies under Dr. Howard Maibach, a prominent dermatologist at the University of California, San Francisco, before accepting a position at NDSU in 1994. (Both mentors continue as collaborators on Singh's work to deliver insulin by skin absorption). Singh passed up lucrative opportunities in the pharmaceutical industry to come to NDSU because he wanted to teach. He felt at ease, because he came from a farming region in India, and quickly developed a rapport with his students. Singh was named teacher of the year three times in the College of Pharmacy, and twice was honored as the college's researcher of the year. This year he received NDSU's Waldron Research Award in recognition of outstanding research achievement. "I have a home here. You can be very quiet and do your job," the industrious Singh says of the atmosphere at NDSU. "People will help you."
One of those people is Dean Webster, a professor in NDSU's Department of Polymers and Coatings, who is advising Singh's team on developing "smart polymer" coatings for microsphere medicines that would be targeted at the heart. (Singh's idea is to have a surgeon inject the medicine between the patient's ribs - alas, skin absorption isn't possible for all that ails humankind.) The goal is to devise a polymer coating that will protect the tiny, tiny spheres of medicine from dissolving until they reach the heart tissue, where they are needed and release medicine at a controlled rate for a longer time. The work is very preliminary, Webster says, but should speed up late this year when the university gets a pair of robots that will help with a wide array of experiments at the university's new nanotechnology center. "We are very excited about that possibility," Singh says of "smart-polymer"-coated micro-spheres. "I hope a lot of good things will be coming out of that."
Oh, he's also working on anticancer microspheres that could be targeted at capillaries in the lungs, and made to release, at a controlled rate, the incorporated anticancer drug at the tumor site. The aim is to increase the concentration of a drug such as Interleukin-2, sparing healthy tissue and thus reducing side effects, while increasing the medicine's effectiveness. Many of the drugs he's working with involve unstable "macromolecules" with short half-lives, making it difficult to control their absorption for optimal effectiveness. It's an arcane but growing field called pharmacokinetics - how drugs are metabolized by the body - and Singh's kinetic energy and optimism have a way of getting under your skin.
-Patrick Springer

































